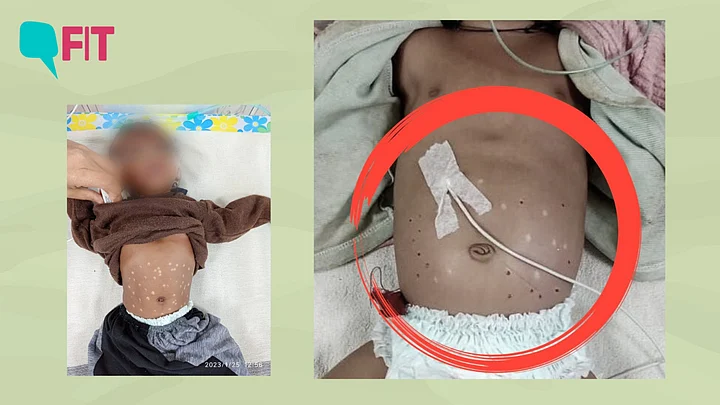
The recent hair-raising news of poking a hot iron rod 51 times in the abdomen of an infant, in a tribal area of Madhya Pradesh's Shahdol, to treat pneumonia shook the collective conscience of the country.
The child, who was suffering from breathing difficulties, died 15 days later in a hospital. In fact, despite being counselled by an Anganwadi worker against it, the mother went ahead with the ‘treatment’.
Surprising as it may seem, similar practices continue across India, more in the rural areas but not unheard of even in urban areas.
For example, covering the newborn’s umbilical stump with cow dung soon after birth has been a very common practice. It has been a major cause of Neonatal Tetanus – a severe, often fatal disease.
Not a One-Off Case
A 2019 study, titled Where Do Mothers Take Their Children For Pneumonia Care? Findings From Three Indian States, shows:
“In the districts of Madhya Pradesh and Uttar Pradesh, most mothers expressed faith in the practice of Jhaad Phoonk or black magic. Such magico-religious practices continued even when the child was treated by other types of care providers.”
Cases such as these have come up time and time again in the last few years. Back in 2006, a three-year-old was branded to cure her of malaria which had resulted in her stomach being swollen.
It repeated in 2015, in Rajasthan’s Rama Kheda village, a four-month-old was hospitalised in critical condition after her stomach was branded with a hot iron to cure her of pneumonia. At the hospital, she was diagnosed with congenital heart disease as well.
The same year, a 40-day-old was hospitalised in Madhya Pradesh’s Ujjain for the same reason.
In 2021, four kids in Madhya Pradesh breathed their last after they were taken to a local 'baba' instead of being rushed to the local hospital.
And it continues in 2023 as well.
Faith-Healing Universe Involves More Than Just Branding
Historically, stories of such inhuman ‘treatments’ are heard more often in reference to mental disorders and epileptic seizures or convulsions due to any cause.
Due to misplaced beliefs from old times, mental health woes have been viewed as signs of demonic possession in some cultures.
As a result, mystic rituals such as exorcisms, ‘jhadas’, physical beating, prayer, and other religious rituals and mumbo-jumbo have been commonly used to 'treat’ the individuals to relieve them from the suffering caused by these disorders.
Faith healers, tantriks, or their equivalent, virtually in every religion, make a living out of ignorance and superstitious beliefs of the community. In a study conducted some years ago in Jaipur by Dr Shiv Gautam, it was shown that more than 2/3rds of mentally ill patients are taken to faith healers before a psychiatrist.
“Faith healing practices include a wide range of activities like performing elaborate rituals, recommending amulets, suggestion for wearing specific rings, branding with rods, chaining in temples, exorcism of jinn and ghosts, animal sacrifices and others.”2014 study titled Ethical Issues Relating to Faith Healing Practices in South Asia: A Medical Perspective
More often than not, people suffering from any mental health conditions in India are taken to faith healers to save them from the evil that’s possessed them. In 2016, newspapers reported about how patients had been “tied to walls with chains cutting through them” in an Allahabad institute.
Why Faith Healing Practices Still Thrive
There are multiple reasons for such practices to thrive.
Illiteracy and lack of education among tribals and rural population living in far flung rural areas in the hinterland is one of the main reasons for these deep-rooted misconceived beliefs.
Abject poverty, and lack of access to even the most basic medical care, compels them to seek relief from these witch doctors.
Educating The Population Might Be The Only Solution
Amelioration of this malady lies in educating the people and strengthening the health infrastructure including setting up of accessible Community Health Centres and Primary Health Centres and equipping these with necessary hardware and facilities.
Above all, healthcare professionals and health care workers like Auxillary Nurse Midwife (ANM) and Lady Health Visitor (LHV) should be given incentives to staff these centres so that these centres become functional in reality and are not merely an entry on paper.
Tribals being well versed in medicinal properties of the local plants and herbs, it may be worthwhile to have Ayush physicians also as part of medical personnel manning these centres. Further, the local populace may be more amenable to the treatment provided by the Ayush physicians as they are more likely to identify with the latter.
Once these centres are staffed adequately and stocked optimally with medicines and other consumables, telemedicine can play a big role in bringing healthcare closer to the people who deserve that the most.
Howsoever abominable certain treatments may look, but it is interesting to note that some of these are prevalent even in the developed western world and research shows that some of these actually work.
Some examples are bee and scorpion sting (venom) therapy for arthritis where the active principle is a compound called Melittin. Maggots have been used for wound healing and medical leeches for venous congestion and blood letting for haemochromatosis.
It is clear that medical procedures and remedies need to be understood in their historical context because the rationale for their use during those times is often very different from the reasons as we understand them today for using them on scientific basis.
(Dr Ashwini Setya is the Adjunct Professor in Gastroenterology, ESIC Medical College, Faridabad, and Senior Consultant with Medanta Institute of Digestive & Hepatobiliary Sciences, New Delhi. Dr Setya is also an advisor and consultant in Medical Law and Ethics. He can be reached at ashwini.setya@gmail.com)