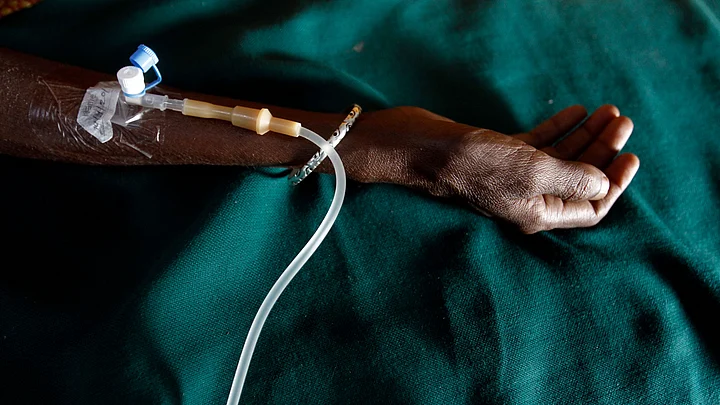
On World AIDS Day 2021, we mark four decades of this mysterious ailment responsible for widespread loss of lives across the globe. We now know this to be a result of the HIV virus, that dramatically lowers the body’s immune defenses.
At the beginning of this century, AIDS-related illnesses (such as all forms of TB, pneumocystis pneumonia in the lungs, cryptococcal meningitis - a painful fungal infection of the brain) were seen among patients unaware of their HIV status, due to lack testing and antiretroviral treatment options. Over 36 million people have died from AIDS-related illnesses since the start of the epidemic.
Over the past five decades, the Indian government has made considerable advances in providing access to testing and antiretroviral therapy (ART) (a cocktail of antivirals drugs that suppress the virus) to People Living with HIV (PLHIV).
Yet, we know that India lost nearly 60,000 PLHIVs in 2019, and there is concern that these numbers could be higher as the pandemic undermines progress, with lockdowns and stretched healthcare systems.
AIDS remains a crisis, and COVID-19 is making it worse, says Winnie Byanyima of the United Nations Programme on HIV and AIDS (UNAIDS). According to UNICEF, 1,20,000 children died from AIDS-related causes, or one child every five minutes in 2020.
As India recovers from the pandemic, World AIDS Day provides an opportunity to assess the response to the continued mortality caused by this crisis.
While there has been a reduction of AIDS-related deaths since 2004, progress has stalled in recent years, highlighting that scale-up of testing and antiretroviral treatment alone is not sufficient to end the epidemic.
Can we do what needs to be done to stop people dying from AIDS?
Maybe – but only if we pay more attention to the people who are most at risk of dying. Close to one-third of PLHIV get linked to HIV programmes when their immune systems are already compromised (CD4 cell counts of less than 200 cells/mm), making them vulnerable to infections. We have also seen PLHIV on antiretroviral treatment develop resistance to their regimen and become vulnerable to life-threatening bacterial and fungal infections: the primary causes of hospitalisation and death among the community.
The World Health Organisation recommends that HIV programmes identify PLHIV at risk of Advanced HIV Disease (technical term for AIDS) to provide a package of prevention, testing, and treatment for the main killer diseases linked to AHD or AIDS.
Yet, several years after the recommendation, screening tests, prevention, and treatment for these life-threatening infections are still missing from HIV programmes in high burden countries like India.
A recent visit to a Médecins Sans Frontières’s (MSF) medical facility, providing hospitalisation for PLHIVs - many of whom have been turned away from other health facilities due to stigma - alarmed me. I witnessed firsthand how people living with HIV in India were in urgent need of critical care due to severe fungal and bacterial infections, just like in the height of the global AIDS epidemic nearly two decades ago.
The COVID-19 pandemic cannot be an excuse to divert attention from HIV. This is not an easy virus to defeat, and we cannot be complacent in our response to the epidemic.
UNAIDS expects governments to reduce the number of people dying from HIV/AIDS to 2,50,000 by 2025; yet this cannot be achieved without throwing a lifeline to people with Advanced HIV Disease.
In India, care models to fit those presenting (and re-presenting) with advanced HIV disease are urgently required. As treatment activists, we need to drive advocacy with the HIV programme to increase access to tests and new medicines. This is crucial for preventing the two major causes of mortality among people living with HIV in India: TB and cryptococcal meningitis.
Most importantly, we need political will from the HIV programme (National AIDS Control Organisation) to reduce the number of deaths among PLHIV, and take the necessary measures to end AIDS.
This article is authored by Leena Menghaney, a lawyer who has contributed to the research and drafting of the HIV/AIDS Act. She is currently a member of the Fight AIDS Coalition (FAC), and works for Medecins Sans Frontieres’ Access Campaign in India.